Autorefraction as an outcome measure of laser in situ keratomileusis
Purpose: To determine the limits of agreement between subjective refraction and autorefraction before and after laser in situ keratomileusis (LASIK) to assess whether autorefraction is a valid refractive outcome measure of refractive surgery.
Setting: Ultralase, Leeds, United Kingdom.
Method: The prospective study involved consecutive preoperative normal patients and post-LASIK patients who had autorefraction using the Nidek ARK 700A autorefractor and careful subjective refraction (masked to autorefraction). Inclusion criteria were age greater than 18 years and healthy eyes with a visual acuity better than 0.1 logMAR (6/7.5) with or without previous LASIK. Refractions were compared by spherical equivalent (SE) using Bland-Altman limits of agreement and astigmatic vector difference using the median and the 95th percentile. The effect of time after treatment and treatment strength were explored.
Results: Data were collected from 208 preoperative patients and 237 post-LASIK patients. Preoperatively, the agreement between subjective refraction and autorefraction for the SE was -0.10 diopter (D) ± 0.35 (SD) and the median difference for the astigmatic vector was 0.28 D with a 95th percentile of 0.72 D. Post-LASIK, the SE agreement was similar, -0.09 ± 0.39 D, but the astigmatic vector agreement decreased slightly with a median of 0.31 D and a 95th percentile of 1.02 D. This decrease reflected poorer agreement in patients whose pre-LASIK refractive error was greater than +4.00 D. Removing this group brought the median astigmatic difference post-LASIK to 0.27 D with a 95th percentile of 0.87 D, similar to that in the preoperative normals. The percentage within ±0.50 D and ±1.00 D of the attempted correction was 56.1% and 78.5%, respectively, with subjective refraction and 51.2% and 78.1%, respectively, with autorefraction.
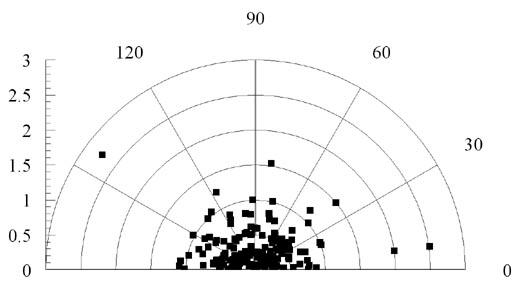
Figure 8 Vectorial display of the difference between subjective and autorefraction for the post-LASIK group. The distance of each marker from the origin indicates the magnitude, with the
position indicating the direction of the discrepancy. No directional bias is evident.
Conclusions: Autorefraction showed excellent agreement with subjective refraction and was unaffected by refractive surgery except after LASIK for high hyperopia. Most outcomes were correctly classified in the standard categories (±0.50 D, ±1.00 D), illustrating that autorefraction is a valid outcome measure of refractive surgery.
Key words: autorefraction, keratomileusis, LASIK, refractive surgery, Ultralase
J Cataract Refract Surg 2004; 30:1921-1928 . 2004 ASCRS and ESCRS
Accepted for publication 22 January 2004.
Konrad Pesudovs PhD
From Ultralase, Leeds, United Kingdom.
![]() Autorefraction after LASIK as PDF (152 Kb)
Autorefraction after LASIK as PDF (152 Kb)
![]()
Index of Papers
[
Welcome ][ Publications ]