An analysis of the astigmatic changes induced by accelerated orthokeratology
Purpose. The change in corneal astigmatism induced by reverse geometry lenses for orthokeratology has not been previously described. This study examines the efficacy of accelerated orthokeratology for reducing astigmatism and whether this varies with the degree of pre-existing astigmatism.
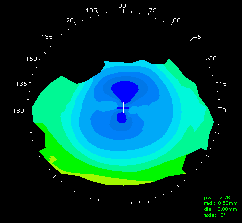
Methods. Twenty-three randomly chosen eyes exhibiting 0.50D to 1.75D pre-fitting with-the-rule astigmatism were retrospectively analysed. Astigmatism was measured by simulated keratometry and corneal topography before and at the completion of a course of orthokeratology. The change in astigmatism measured by keratometry was calculated by two vector analysis techniques: the Bailey-Carney method which was designed for contact lens induced corneal shape changes and the Alpins method which was designed for surgically induced corneal shape changes. The change in astigmatism measured by corneal topography was calculated by the Eyesys Version 3.2 software.
Results. Most (20/23) patients had some reduction of astigmatism, but orthokeratology is incapable of a total elimination of pre-fit astigmatism. Alpins vector analysis showed that an increased efficacy of 60 to 80% would be required to eliminate astigmatism. All three methods found a 50% mean reduction in astigmatism from the pre-fit level. Topographical analysis indicates that the reduction in astigmatism occurs mainly over the central 2.00 mm chord. There is a very poor correlation between the pre-and post-wear corneal astigmatism at the 2.00 mm chord (R2 = 0.11, p = 0.04) and the predictability of the final astigmatic axis is also poor (Angle of Error-1.22 SD. 27.35).
Conclusions. Accelerated orthokeratology seems more successful at reducing with-the-rule astigmatism than conventional orthokeratology. However, it only reduces pre-existing astigmatism by an average of 50% and it does not do so reliably neither for magnitude nor direction. These results provide two useful patient selection criteria for orthokeratology: 1) Assuming 0.50D to 0.75D of astigmatism is a satisfactory outcome, then orthokeratology can be expected to be successful for pre-fitting astigmatism of up to 1.00D to 1.50D. 2) The greater the pre-existing astigmatism, the less likely orthokeratology is to be successful.
Clin Exp Optom 2002;85(5)
John Mountford DipAppSc FAAO FVCO FCLS
Suite 6, 18th Floor, 141 Queen St, Brisbane 4000, Queensland, Australia
Konrad Pesudovs BScOptom PhD DipAdvClinOptom MCOptom FAAO FVCO FCLSA
Department of Ophthalmology, Flinders Medical Centre and Flinders University of South Australia, Bedford Park 5042, South Australia, Australia
EyeSys as GIF (30 Kb)
![]()
Index of Papers
[ Welcome ][ Publications ]

